QUESTION: A 58 year-old right hand dominant admin officer complains of pain at the base of her thumb when opening jars, turning keys, writing and knitting. She is worried that she is developing arthritis, and remembers how debilitated her mother was with arthritis in her hands. Is there a role for hand therapy?
What is it?
Osteoarthritis at the base of the thumb is a degenerative condition, which may be associated with pain, stiffness, weakness and increasing deformity. Symptoms can be aggravated by activities requiring strong pinch or sustained gripping activities. The thumb may look swollen and be tender to touch, and ache after prolonged activities. Particular aggravating activities include opening jars, turning keys, writing, pinching pegs or leaning on an extended wrist.
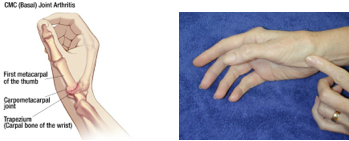
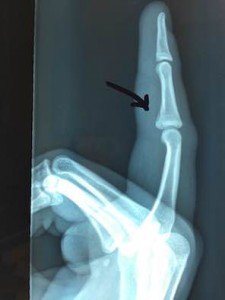
Location of pain at the base of the thumb
Clinical Examinations
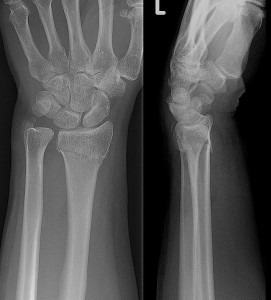
An X-Ray may be helpful to determine the degree of degenerative change, although symptoms don’t necessarily correlate with severity of X-ray change.
Treatment
Most people with arthritis at the base of the thumb will respond well to a custom made splint, and instruction in various self-help strategies with an appropriate exercise program. Your hand therapist will provide you with:
- Education about appropriate care of your painful thumb
- Appropriate exercises to improve your movement, control, and ability to perform activities of daily living
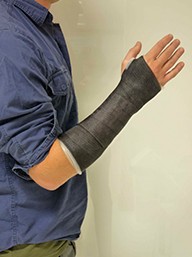
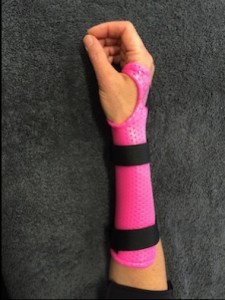
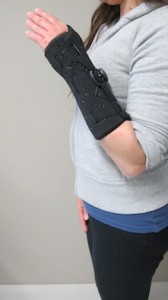
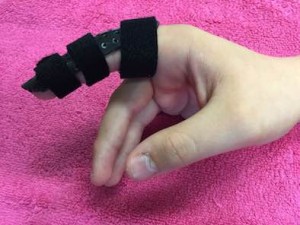
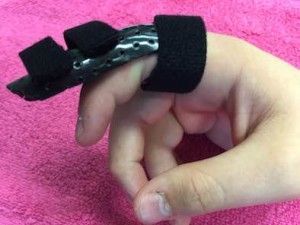
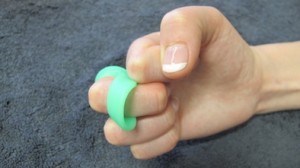
- A supportive splint to rest the thumb, to allow you to perform activity without pain. The splint may be made from a soft neoprene material or custom made out of thermoplastic materials
- Neuromuscular and graded strengthening exercises when appropriate
- Neural glides

Push Brace
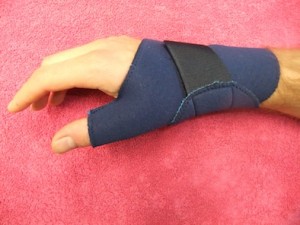
Neoprene thumb and wrist brace
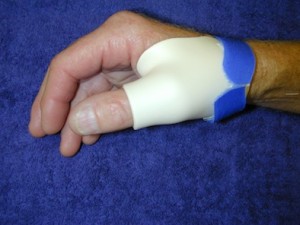
Short opponents splint
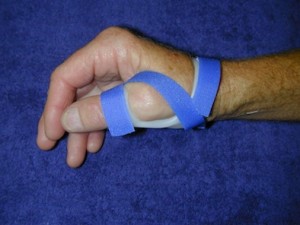
Three point thumb splint
Surgical Treatment
Surgical review may be required depending on your response to conservative treatments. Your therapist will be happy to discuss with you and your GP whether referral to a hand surgeon is appropriate.
If you have any questions regarding a condition you have or to book an appointment, feel free to contact us here. We’d be more than happy to help.